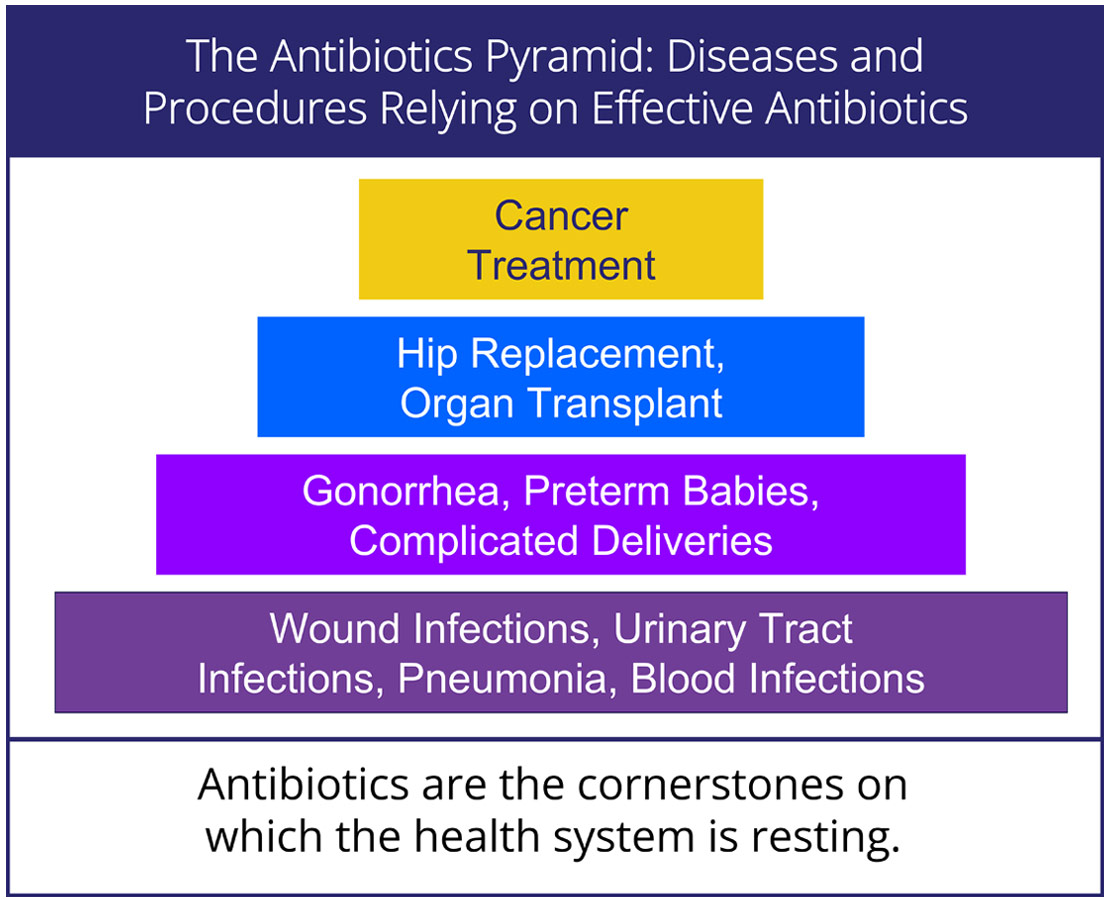
AMR occurs when germs like bacteria, viruses and fungi evolve in ways that make the medicines used to treat them stop working. These germs can then cause resistant infections that can be difficult and sometimes impossible to treat.1

By 2050, it is estimated AMR will cause more deaths than cancer unless concerted efforts are undertaken to counter its progression. 3